MOLES OR NAEVI

What causes naevi?
When do naevi appear?
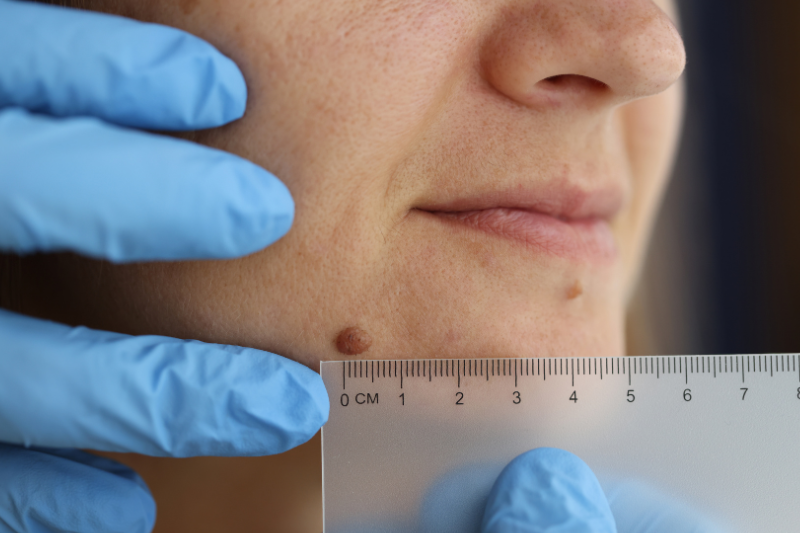
What happens to naevi in the course of a lifetime?
Generally an indivudual naevus grows slowly over many years and ultimately attains its full size and then remains stable for decades. Eventually many naevi regress such that very few true moles are present in the 7th and 8th decades.
As we age, new naevi are rare and that is why a growing lesion in an adult has a greater risk of being a melanoma.
Sometimes the body’s own immune system “attacks” a mole. An area of depigementation (whitening) occurs around the mole and ultimately the mole may disappear. This clinical picture of a mole with a surrounding pale ring is termed “halo naevus”.
There is a huge range as to what is considered a normal number of moles. In studies of fair skinned Australians, in the third decade of life, the average number of moles per person is 35.
